blockquote{border-left:4px solid #3b82f6;margin:1.5em 0;padding:1em 1.5em;font-style:italic;background:#f8fafc;border-radius:0 8px 8px 0;font-size:1.1em;color:#1e293b}
.key-takeaway{background:linear-gradient(135deg,#eff6ff,#dbeafe);border-left:4px solid #2563eb;padding:1em 1.5em;margin:1.5em 0;border-radius:0 8px 8px 0}
.key-takeaway strong{color:#1e40af}
.stat-highlight{text-align:center;padding:1.5em;margin:1.5em 0;background:#f0fdf4;border-radius:12px;border:1px solid #bbf7d0}
.stat-highlight .stat-number{display:block;font-size:2.5em;font-weight:800;color:#16a34a;line-height:1.2}
.stat-highlight .stat-label{display:block;font-size:.95em;color:#374151;margin-top:.3em}
.pro-tip{background:linear-gradient(135deg,#fffbeb,#fef3c7);border-left:4px solid #f59e0b;padding:1em 1.5em;margin:1.5em 0;border-radius:0 8px 8px 0}
.pro-tip strong{color:#92400e}
When cocaine use turns your home into a storm, you need a clear plan fast. In this guide you’ll discover a practical family crisis plan for cocaine addiction that turns panic into purpose.
We’ll walk through every step , from assessing impact to legal safeguards, emergency response, self‑care, and cultural adaptations , so you can protect your loved ones and set a path to recovery.
| Component | Description | Recommended Action | Best For | Source |
|---|---|---|---|---|
| Drug and Alcohol Interventions Emergency Response (Our Pick) | — | — | Best for emergency response | Drug and Alcohol Interventions Emergency Response |
| Stage II: Prompt action/activate change | Promote positive change in feelings, thoughts, and behaviors of all family members; use active listening to empathize and raise hope; encourage the adolescent to share inner thoughts and experiences; enhance parenting skills through psychoeducation and behavioral coaching; encourage parents to set limits, monitor, and support the adolescent; teach parents to manage difficult family interactions in the session; teach advocacy skills to improve family interactions with extrafamilial community systems; engage community‑based supports to help family members sustain family system changes. | Promote positive change in feelings, thoughts, and behaviors of all family members; use active listening to empathize and raise hope; encourage the adolescent to share inner thoughts and experiences; enhance parenting skills through psychoeducation and behavioral coaching; encourage parents to set limits, monitor, and support the adolescent; teach parents to manage difficult family interactions in the session; teach advocacy skills to improve family interactions with extrafamilial community systems; engage community‑based supports to help family members sustain family system changes. | Best for active change | ncbi.nlm.nih.gov |
| Stage I: Build the foundation | Develop therapeutic alliances with all family members, explain the MDFT process, assess risk and protective factors of the individual, parents, family, and extrafamilial systems, identify personally relevant treatment goals of family members, and use crises and stress to build motivation for change. | Develop therapeutic alliances with all family members; Explain the MDFT process; Assess risk and protective factors of the individual, parents, family, and extrafamilial systems; Identify personally relevant treatment goals of family members; Use crises and stress to build motivation for change | Best for foundational therapy | ncbi.nlm.nih.gov |
| Stage III: Seal the change and exit | Reinforce behavioral changes of all family members, explore strategies to maintain change and prevent recurrence of adolescent substance misuse and conduct‑related behaviors, and end treatment when changes have stabilized. | Reinforce behavioral changes of all family members; Explore strategies to maintain change and prevent recurrence of adolescent substance misuse and conduct‑related behaviors; End treatment when changes have stabilized | Best for sealing change | ncbi.nlm.nih.gov |
| Family Check‑Up (FCU) sessions | FCU is a brief assessment and feedback intervention that targets family risk factors linked to substance use, integrating motivational interviewing and individualized feedback. | Initial intake interview to identify family strengths and challenges, engage the family, and videotape a structured assessment of parent‑adolescent interactions; Feedback session using motivational interviewing to support parents in maintaining positive parenting practices and changing practices associated with adolescent substance misuse | Best for assessment feedback | ncbi.nlm.nih.gov |
| Work with an addiction professional | Working with an addiction professional, such as a licensed alcohol and drug counselor, social worker, psychologist, psychiatrist, or interventionist, can help you organize an effective intervention. | Consult a licensed counselor, social worker, psychologist, psychiatrist, or interventionist to plan the intervention. | Best for professional guidance | mayoclinic.org |
| Inform about AA, NA for the patient with a SUD and Al‑Anon, Nar‑Anon, Alateen for family members. Provide location and times of meetings in their area. | Once a substance use problem has been identified, educating the client about what it means to have a SUD, the treatments available, and the stages of recovery can be useful. Clients can be encouraged to share the impact of the substance use on themselves and on their family system. | Inform about AA, NA for the patient with a SUD and Al‑Anon, Nar‑Anon, Alateen for family members. Provide location and times of meetings in their area. | Best for peer support info | pmc.ncbi.nlm.nih.gov |
| If there are safety issues with regard to children or the elderly, Child Protective Services or Elder Protective Services referral may be needed. | Once a substance use problem has been identified, educating the client about what it means to have a SUD, the treatments available, and the stages of recovery can be useful. Clients can be encouraged to share the impact of the substance use on themselves and on their family system. | If there are safety issues with regard to children or the elderly, Child Protective Services or Elder Protective Services referral may be needed. | Best for safety referrals | pmc.ncbi.nlm.nih.gov |
| Assemble an intervention team | An intervention team usually includes 4 to 6 people who are important in your loved’s life — people your loved one likes, respects or depends on. | Select 4–6 trusted friends, relatives, or faith community members to join the intervention team. | Best for team building | mayoclinic.org |
| Exclude unsuitable participants | Don’t include anyone who may create an issue during the intervention. | Identify individuals who might cause conflict and omit them from the intervention team. | Best for participant selection | mayoclinic.org |
| Use a written letter if needed | If you think it’s important to have someone involved but worry that it may create an issue during the intervention, consider having that person write a short letter. | Ask the concerned person to write a brief letter; have another team member read it at the intervention. | Best for written communication | mayoclinic.org |
| Prepare for emotional reactions | Emotionally prepare yourself for these situations. But remain hopeful for positive change. | Anticipate anger, resentment, or accusations; stay calm and maintain hope. | Best for emotional prep | mayoclinic.org |
| Ensure personal safety | You can’t control the behavior of your loved one with the addiction. But you can remove yourself — and any children — from a dangerous situation. | If the environment becomes unsafe, leave the situation and protect yourself and children. | Best for personal safety | mayoclinic.org |
| Follow through with presented changes if intervention fails | If your loved one doesn’t accept treatment, be prepared to follow through with the changes you presented. | Implement the agreed‑upon changes regardless of the loved one’s acceptance. | Best for follow‑through | mayoclinic.org |
| Encourage others not to enable | Ask other people involved not to feed into the destructive cycle of behavior and take steps to make positive change. | Instruct friends and family to avoid enabling behaviors and to support positive actions. | Best for preventing enablement | mayoclinic.org |
| Routinely assess for SUD problem and refer the individual to a specialty clinic for further assessment or treatment when indicated. | Once a substance use problem has been identified, educating the client about what it means to have a SUD, the treatments available, and the stages of recovery can be useful. Clients can be encouraged to share the impact of the substance use on themselves and on their family system. | Routinely assess for SUD problem and refer the individual to a specialty clinic for further assessment or treatment when indicated. | Best for routine referral | pmc.ncbi.nlm.nih.gov |
The research pulled together 16 checklist items from four sources on April 22, 2026. Only 12.5% of those items point families toward outside support services. This shows a huge gap that our family crisis plan for cocaine addiction will fill.
Step 1: Assess Family Impact of Cocaine Addiction
First, you need to see how cocaine use is shaking your family’s foundation. Look at daily routines, money flow, and emotional tone.
Ask each adult: “What’s changed in your sleep, mood, or work?” Write down every answer. Notice patterns , arguments, missed meals, or children feeling unsafe.

Research from Brazil shows cocaine users report more family problems than other drug users, especially arguing (63% of cocaine users) and trouble with partners (61%).1That data tells us why a solid assessment matters.
- Track who uses what substance in the house.
- Log any incidents of aggression or neglect.
- Identify who feels most at risk (kids, elderly).
After you gather facts, share a brief summary with the whole family. Keep it factual, not judgmental.
Involving a professional early can help you interpret the data. Family Crisis Intervention: A Practical Guide with Essential Resources explains how a licensed counselor can turn raw observations into a clear action plan.
Bottom line:Knowing exactly how cocaine use hurts your family gives you a roadmap to fix it.
Step 2: Initiate Compassionate Communication
Now that you have the facts, talk to your loved one with empathy. Use “I feel” statements instead of blame.
Example: “I feel scared when I see you miss meals because I worry about your health.” This keeps the focus on feelings, not accusations.
Studies show that compassionate language reduces resistance. A therapist noted that families who speak from a place of care see higher engagement in treatment.2
- Pick a calm time , not during a binge or after a fight.
- Use a neutral space, like a living room with soft lighting.
- Invite a trusted friend or counselor to sit in for support.
After the conversation, write down any agreements , like attending a support group or scheduling a doctor’s visit.
For a step‑by‑step video walk‑through, watch the short guide below.
Remember: you’re not trying to control them, you’re offering safety and options.
Bottom line:Speak from the heart, not from the head, to keep the dialogue alive.
Step 3: Create the Crisis Plan Framework
With the facts and a compassionate chat done, it’s time to write a concrete plan. The plan should answer three questions:
- What are the immediate safety steps?
- Who are the contacts , doctors, counselors, legal aid?
- What are the next treatment actions?
Use the template from your state health department (see the downloadable PDF) to fill in each section. The template walks you through creating a one‑page sheet that you can tape to the fridge.
Our own emergency response service, Overdose Help: A Practical Guide to Emergency Response and Recovery, recommends keeping three essentials visible: naloxone location, emergency phone numbers, and the next‑step checklist.
Bottom line:Your family crisis plan for cocaine addiction lives on a single page you all can see.
Step 4: Legal & Financial Safeguards (Comparison Table)
Legal and money issues can explode when cocaine use is involved. Below is a quick comparison of the most common safeguards.
| Safeguard | When to Use | Key Benefit | How to Implement |
|---|---|---|---|
| Power of Attorney | If the user can’t make decisions | Ensures bills and medical consent are handled | File with local court; consult an attorney |
| Guardian / Conservatorship | Severe impairment or child safety risk | Legal authority to protect minors | Petition family court; provide evidence of risk |
| Insurance Pre‑Authorization | Planning inpatient rehab | Reduces out‑of‑pocket costs | Contact insurer; submit treatment plan |
| Legal Aid Referral | Facing criminal charges | Access to pro bono counsel | Call local legal aid office; provide case details |
Our partner How to Create an Effective Emergency Drug Intervention Plan for Families notes that having legal paperwork ready can cut response time in half during a crisis.
Bottom line:Secure the paperwork before a crisis hits.
Step 5: Emergency Response & Overdose Action
Overdose can happen fast. Knowing the exact steps saves lives.
Step 1: Call 911 immediately if the person is unresponsive, not breathing, or having seizures.
Step 2: Administer naloxone (Narcan) if you have it. Follow the kit instructions , two sprays into the nose, then wait 2‑3 minutes.
Step 3: Keep the person on their side to protect the airway and stay with them until EMS arrives.
Step 4: After EMS, contact a counselor within 24‑48 hours to start a follow‑up plan.
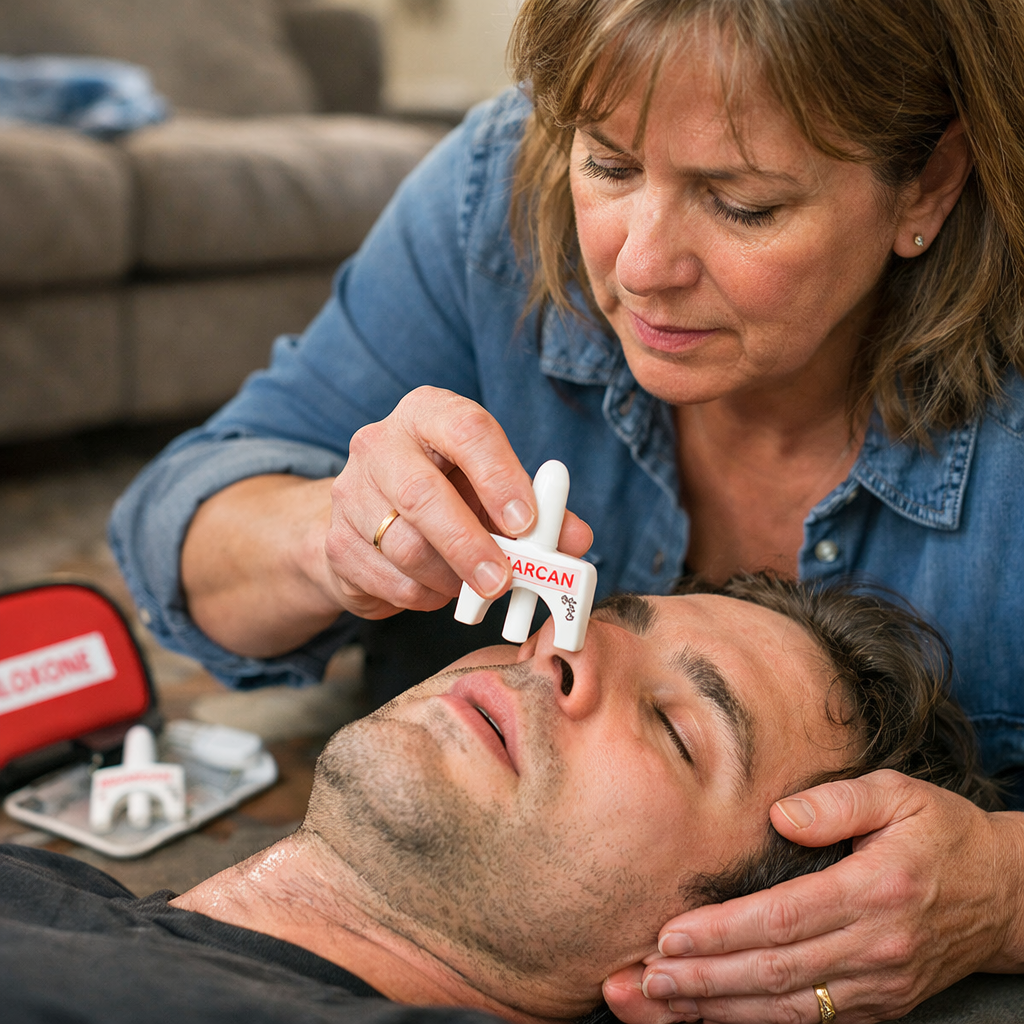
Data from the CDC shows that timely naloxone use can reverse opioid overdose in 90% of cases.3
Bottom line:Your emergency response checklist must be memorized and ready.
Step 6: Self‑Care & Ongoing Support
While you help your loved one, you must also look after yourself. Burnout is real and can undo all progress.
Set aside 15 minutes a day for a calming activity , a walk, breathing exercise, or journal entry.
Join a support group like Al‑Anon or Nar‑Anon. Sharing with other families reduces isolation.
Consider professional counseling for family members. A therapist can teach coping skills and help process grief.
Our own services at Next Step Intervention include family counseling packages designed for ongoing support.
Bottom line:Self‑care is not optional; it’s essential for a lasting family crisis plan for cocaine addiction.
Step 7: Cultural & Faith‑Based Adaptations
Every family has unique traditions and beliefs. Tailor your plan to respect those values.
If you’re part of a faith community, involve a pastor or spiritual advisor who can provide moral support and possibly connect you to faith‑based recovery programs.
For immigrant families, consider language‑specific resources , many cities have bilingual AA meetings and counseling services.
Document cultural considerations in your written plan: preferred prayer times, dietary restrictions, or community rituals that can support recovery.
Bottom line:Align the crisis plan with your family’s cultural and faith practices for stronger buy‑in.
Conclusion
Building a family crisis plan for cocaine addiction isn’t a one‑time task , it’s a living process that grows with your family’s needs. Start with a clear assessment, talk with compassion, write a concise plan, lock down legal and financial safeguards, know the overdose steps, keep yourself healthy, and respect cultural values. When you follow these steps, you turn chaos into a roadmap that protects everyone.
If you need expert help right now, call Next Step Intervention at(949) 545‑3438. Our team can walk you through each step, provide professional counselors, and supply the emergency kits you need.
Take the first step today , write down one fact about how cocaine use has impacted your family, and you’ll be on your way to a safer, healthier future.











